Although it is painless and impossible to transmit to others, tinea versicolor often causes great distress in patients. Sometimes referred to as pityriasis versicolor, this fungal infection causes skin discolorations that can be embarrassing, especially since it is most common in teenagers. Though most frequent in young adults, the condition can affect anyone and is quite common in tropical areas. It leaves behind no lasting effects, however, and is usually easy to treat. Here are a few ways one can successfully treat and prevent this infection.
General Info on Tinea Versicolor
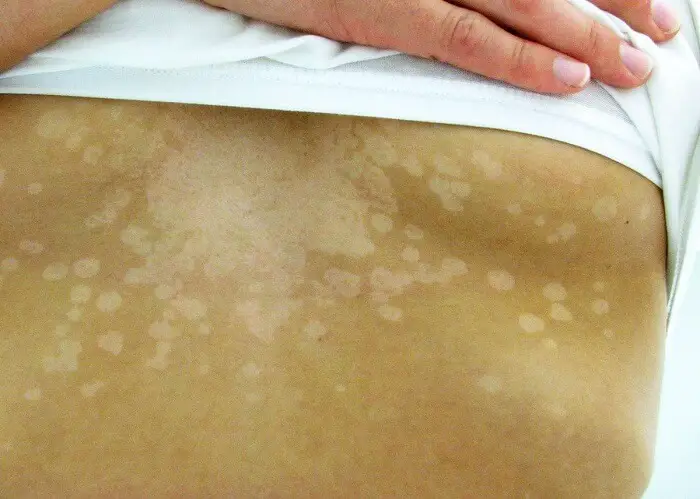
Tinea versicolor is a superficial fungal infection of the skin that appears as an area of discoloration. This infection changes the color of the skin and may cause scaling but creates no other problems. It is most often found on the shoulders, back and chest although it can appear anywhere. Sometimes tinea versicolor occurs in skin folds, affecting skin in the groin, under the breasts and inside elbows or knees.
The infection rarely affects the face, but facial skin infections aren’t impossible. People experience this condition regardless of skin color, gender or age, but the condition is most often found in teenagers and more likely in males than females. Facial symptoms are most likely to occur in those of African-American descent.
Signs and Symptoms of Tinea Versicolor
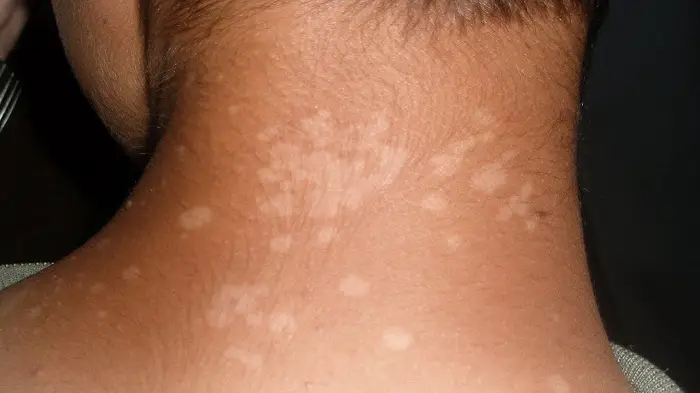
The most common symptom of tinea versocolor is discolored patches of skin that may look like a rash. The affected skin can be darker or lighter than the surrounding skin but will not respond to a suntan the way other skin does. Patches of tinea versicolor are typically brown, white, pink or red. Some patients also experience slight itching at the affected site as well as mild skin scaling.
Tinea versicolor symptoms commonly appear when the weather is hot and humid, sometimes disappearing on their own when the weather cools. Discolored skin patches can also appear during cool weather and become more pronounced or bothersome as the weather grows warmer. People who live in tropical climates may experience these symptoms year-round without any significant changes in their condition. Those living in the more northern parts of the globe are far less likely to encounter tinea versicolor.
Causes of Tinea Versicolor
Tinea versicolor is caused by the yeast family Malassezia, which contains 14 known species. This yeast is natural and is commonly found on human skin. The discoloration of tinea versicolor occurs when the yeast experiences a burst of growth. Malassezia yeast produces a chemical known as azelaic acid. When too much yeast is present, the corresponding increase in azelaic acid overcomes and irritates the skin, causing the discoloration and scaling.
Conditions that increase the growth rate of yeast include the following:
- Hot and humid weather conditions.
- Oily skin.
- A compromised immune system.
- Hormonal changes.
Comprehending the causes of tinea versicolor make it easy to understand why teenagers and young adults are most commonly affected. Hormonal changes are common in teens and often create oily skin conditions in which Malassezia yeast thrive.
Tinea Versicolor Diagnosis and Treatment
The diagnosis of tinea versicolor is a simple process that involves examining a skin scraping underneath a microscope. If large amounts of yeast are present on the slide, tinea versicolor is to blame for the patient’s skin problems. It is also possible to confirm a tinea versicolor diagnosis with an ultraviolet light known as a Wood lamp. The skin rash will appear a fluorescent yellow-green color if tinea versicolor is to blame for the rash. Upon visual examination, tinea versicolor resembles both eczema (pityriasis alba) and vitiligo, so a skin scrape or Wood lamp test are often required for a proper diagnosis. Fungal cultures are very difficult to grow in the lab, making them an ineffective diagnostic tool for this condition.
Unlike other skin conditions, tinea versicolor does not cause severe itching, lumps, hair loss, skin ulcerations or swollen lymph nodes. The presence of these symptoms rules out a tinea versicolor diagnosis.
Once tinea versiclor is confirmed, treatment involves the application of an anti-fungal agent. The Mayo Clinic suggests the application of shampoos, gels, creams and lotions that contain 2.5 percent selenium sulfide or ketoconazole. If tinea versicolor is present on a large area of the body or frequently returns, oral anti-fungal medications such as itraconazole and fluconazole may also be helpful. Resistant and abnormal cases should be referred to a dermatologist.
Although the yeast that causes the issue is easy to kill, the skin discoloration associated with tinea versicolor often lasts for weeks to months. It will clear completely, but it’s important for patients to understand that clear skin will take time. Patients who don’t see a change in their skin may prematurely discontinue treatment, believing it to be ineffective.
Preventing Tinea Versicolor
Because there is no way to remove all yeast from the skin, tinea versicolor frequently returns in patients who have experienced it before. To prevent this, the same anti-fungal medications and creams used to treat the condition may be used once or twice a month. Patients can also change their home care routine to prevent an outbreak.
To reduce the risk of tinea versicolor, patients should stay away from oily skin care products. A daily application of sunscreen with an SPF of 30 or higher is recommended but only with a non-greasy, oil-free formula. Preventing tans and sunburns reduces the risk of tinea versicolor and makes an outbreak less visible. During warm weather, wear loose, breathable clothing to avoid excessive sweating. Cottons and linens work best.
The Bottom Line
Tinea versicolor is not contagious, causes no pain and is easy to treat with anti-fungal agents. Patients experience no lasting ill effects from the condition but may need to deal with frequent relapses throughout their lives. Preventing the condition involves reducing the amount of oil and sweat present on the skin so that the yeast which causes the problem doesn’t experience growth spurts.
